By Becca Taurisano
Thursday, April 22, 2021
When the Dorothy G. Griffin Radiation Oncology Center opened in Oneida in July 2019, it eliminated the need for Central New Yorkers to leave the region for high-quality radiation treatment. As a member of the Roswell Park Care Network, the new center provides Roswell Park Comprehensive Cancer Center’s stringent approach to quality.

In 2016, Oneida Health set out to build a first-class oncology program. From the beginning, they knew one factor mattered more than any other: delivering an unmatched approach to quality. To achieve this, Oneida Health partnered with Roswell Park Comprehensive Cancer Center.
Roswell Park Comprehensive Cancer Center, based in Buffalo, is ranked No. 14 nationally in cancer care by the 2020–2021 US News & World Report, putting them among the top 1.5% in the nation for comprehensive cancer centers. Roswell Park is the only hospital system in Upstate New York to be recognized in 2020–2021. They are also the only National Cancer Institute (NCI) Designated Comprehensive Cancer Center in Upstate New York. NCI is the highest federal rating a cancer center can achieve in recognition of their innovative research and leading-edge treatments.
As a member of the Roswell Park Care Network, Oneida Health brings the services of Roswell Park to Central New York.
“Everyone deserves convenient access to the best care possible,” says Gene Morreale, President and CEO at Oneida Health. “Our affiliation provides the impact of Roswell Park’s comprehensive cancer services through pathway care plans developed with the expertise of their world-renowned physicians. Together with our onsite full-time Roswell Park Physicians and highly trained staff, we are able to provide patients with access to some of the latest treatment options from a nationally ranked cancer center.”
The most recent addition to Oneida Health’s Cancer Care program is the newly constructed 6,000 sq. ft. Dorothy G. Griffin Radiation Oncology Center. Maya Mathew, MD, a Roswell Park radiation oncologist, is the full-time Medical Director of the center. As a child growing up in Kerala, India, Dr. Mathew knew she wanted to pursue a career in oncology when her aunt was diagnosed with cancer. After coming to the United States, Dr. Mathew completed a surgical internship at Penn State and residency at Loyola University Medical Center in Chicago. Later on, while practicing radiation oncology for nearly three years at Memorial Hospital in Gulfport, she was struck by the number of advanced cancer patients she was seeing, particularly young patients. Mathew knew she wanted to be affiliated with a NCI-designated cancer center so she could actively focus on promoting awareness of cancer prevention, early detection and treatment in the community, which is what drew her to Roswell Park.
“I was frustrated seeing advanced cases in a semi-rural area when I practiced. Now, I am able to bring Roswell-quality comprehensive cancer care, No. 14 in the nation, and No. 2 in New York State, to the people of Central New York,” Dr. Mathew says. “When you are fighting the side effects of cancer treatment, it is helpful for the patient to receive treatment locally. Patients receive the same quality of care here close to home as they would at the main center in Buffalo. That is the uniqueness of our program. We provide the full Roswell experience.”
From treatment planning, to peer review, quality assurance and treatment delivery, the center’s approach is designed to deliver the same quality of care that is provided in Buffalo. Throughout the process, Dr. Mathew and her team rely on the research backing and clinical expertise of Roswell Park in Buffalo.
“All protocols, whether medical oncology or radiation oncology in Oneida, are common across Roswell Park physicians,” Dr. Mathew says.

Maya Mathew, MD, Medical Director of Radiation Oncology
Planning Tailor-Made Treatment
In treatment planning, the goal is to always preserve as much healthy tissue as possible using the ALARA (as low as reasonably achievable) approach to radiation dosages, while still effectively treating the cancer site and achieving the best patient outcome. During the treatment planning phase, Dr. Mathew conducts anatomical contouring using CT images, which is both an art and a science to treatment planning.
“We determine what to treat and what to spare,” Mathew says. “Radiation therapy is not a recipe that can be followed for everyone. We are providing personalized treatment plans. It is more of a tailored approach.”
Using an onsite CT simulator, Dr. Mathew and her team use advanced imaging techniques and software to deliver precise dosages while taking every measure to minimize the exposure to healthy tissue. In some cases, Dr. Mathew can also take advantage of other imaging modalities including a new PET/CT and 3 Tesla MRI available at Oneida Health to fuse images for more invasive tumors.
When more complex cases are presented at the center, Dr. Mathew has the advantage of Roswell Park’s tumor board. The tumor board is a multidisciplinary team of Roswell Park medical and radiation oncologists, radiologists, pathologists and surgical oncologists who are among the best in the nation. This team ensures that the treatment plan is the right one.
“Roswell is a comprehensive cancer center, so we can lean on our team to come up with the most appropriate plan,” Dr. Mathew says. “This is particularly beneficial to the patients as they benefit from their specialized expertise. That is the beauty of collaborating with a comprehensive cancer center.”
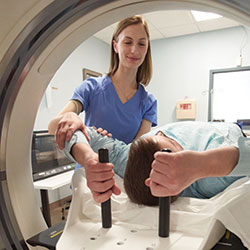
Patients benefit from on-site simulation CT and advanced imaging located conveniently on campus. Rossi is pictured.
Peer-Review by Disease-Site Specialists
Once a treatment plan has been designed by Dr. Mathew, it is presented at a peer-review conference where all the Roswell park radiation oncologists examine the treatment plan. This process is adhered to for every patient. The peer-review board has disease-site specialists who perform a rigorous review of every proposed treatment plan across Roswell Park’s outpatient network. The board dissects the plans, ensures that all dose limits are met, field arrangements are optimal, comorbidities are properly considered and makes any suggestions for improvement.
“The board is made up of different radiation oncologists who treat specific disease sites, so I’m getting the expertise from specialized physicians who are reviewing my treatment plans,” Dr. Mathew says. “That is an assurance for the patient and the referring providers that they are getting the best possible care.”

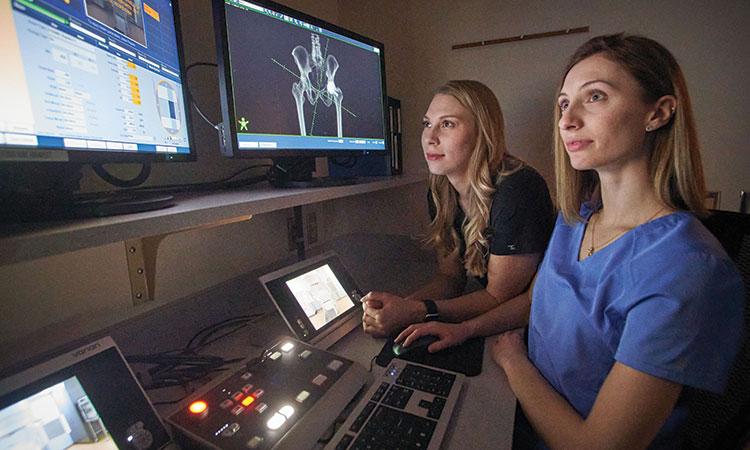
During the treatment planning phase, Dr. Mathew and Roswell Park Dosimetrist, Vanessa Rundle, MS, CMD, RT(R)(T), conduct anatomical contouring using CT images, which is both an art and a science to advanced treatment planning.
Quality Assurance for Every Patient
Once the peer-review board has ensured a plan meets Roswell Park safety protocols and provides the best approach to treatment, an onsite Roswell physicist performs end-to-end quality assurance tests. The quality assurance conducted by the physicist validates the treatment plan will be delivered as prescribed. If any part of the plan does not meet Roswell standards, treatment will not be administered and the plan will be reevaluated. This process is performed for every patient receiving care at the center.
“The quality assurance piece with the help of our physics team is essential. They have their protocols to follow and if the plan does not adhere to Roswell standards, the plan will not be approved to roll out,” Dr. Mathew says. “It is a long process but in the end the patient can be assured that they receive the best care.”
In addition to internal quality assurance, the center also participates in third party review to further validate the quality of treatment plans being delivered. The review is completed by the MD Anderson Imaging and Radiation Oncology Core (IROC) Quality Assurance Center in Houston, Texas.
The center is equipped with TrueBeam radiotherapy, the most advanced linear accelerator and radiosurgery treatment system available. Pictured from left to right: Meghann Wright, RT(T), and Rossi
Excellence in Treatment Delivery
At Oneida Health, the quality of cancer treatment delivery is a combination of state-of-the-art technology and staff expertise. Radiation therapists use a TrueBeam linear accelerator to generate and deliver precise photon beams to tumors in the body, as well as Stereotactic Beam Radiation Therapy (SBRT) to deliver a course of therapy in a condensed timeframe. Radiation therapists also employ motion management (RGSC- Respiratory Gating for Scanners), DIBH (Deep inspiration breath hold), and prone breast radiation therapy techniques to reduce unnecessary radiation doses to healthy organs.
“We have cutting edge treatment systems here in the building so the patient does not have to go anywhere else. But the expertise of the staff, in the field of cancer care, is the difference,” Dr. Mathew says.
Oneida Health staff are also trained to educate the patient about what treatment they are getting and why, making the patient a partner in the treatment they receive and providing them with comfort along the way.
“Each cancer patient is close to my heart,” Dr. Mathew says. “Walking them through their treatments to completion, and achieving the best patient outcome; that is most rewarding for me. The patient experience is an essential ingredient to the delivery of a quality treatment plan.”

Collaboration of a highly skilled team of employees is the difference in providing and meeting stringent quality treatment measures at the center. Pictured left to right: Kare Nicholas, RN, BSN, and Chief Radiation Therapist/Radiation Oncology Center Manager Shaun Maroney, RT(T), MHA
Cohesive Patient Care
Patients and providers who choose Oneida Health will also benefit from the collaboration and continuum of care between medical oncology, radiation oncology and the imaging centers on campus. The William L. Griffin Medical Oncology Center, which opened in 2017, offers 12 infusion suites, a hematology/oncology outpatient office and is directed by a Roswell Park-affiliated physician who provides evaluations, chemotherapy infusions, palliative medicine, hematology, nutrition services, and several cancer screening services. As part of a three phase plan to oncology, Oneida Health has also invested in the expansion of their imaging, which now includes a 3 Tesla MRI, CT Simulation, PET/CT, nuclear medicine camera and a second 3D mammography machine.
“This cohesive, high-quality cancer care program was the singular vision of the Roswell Park and Oneida Health partnership from the start,” Morreale says. “Because of valued relationships with the Griffins and Gormans, as well as Roswell Park, we can now provide the very best cancer care to Central New Yorkers right in Oneida.”
For more information about Radiation Oncology at Oneida Health, visit oneidacancer.org.






 “There has always been support 100% of the time for every emergency case, and it’s a huge responsibility for us to be able to provide the kind of care we provide to the community. It is a privileged role we have, and I feel fortunate that we are fully supported to take care of our patients and make sure they get the best treatment possible.”
“There has always been support 100% of the time for every emergency case, and it’s a huge responsibility for us to be able to provide the kind of care we provide to the community. It is a privileged role we have, and I feel fortunate that we are fully supported to take care of our patients and make sure they get the best treatment possible.”













 Matthew Chaffin, MD, Compliance Officer
Matthew Chaffin, MD, Compliance Officer



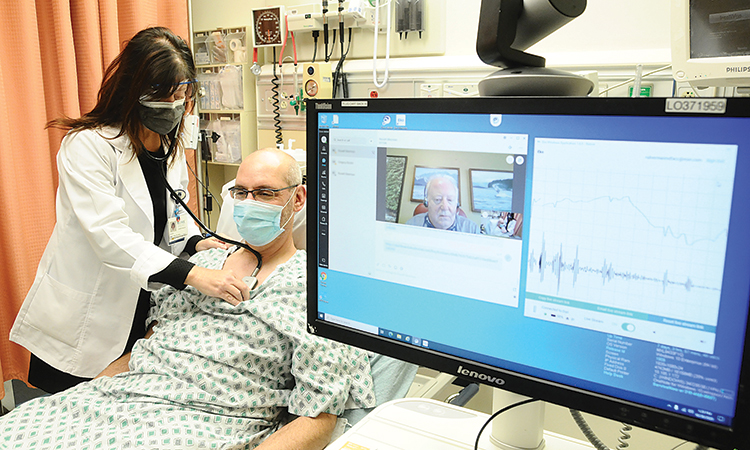
 Bluetooth stethoscope
Bluetooth stethoscope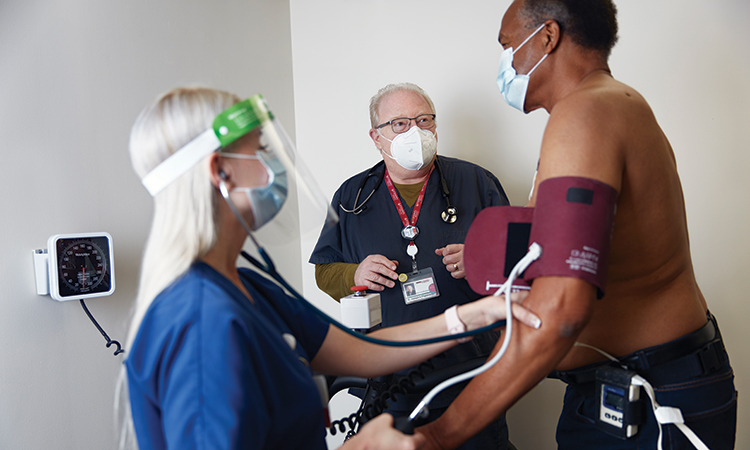




 Ruham Nasany, MD, is leading a multi-disciplinary team for the new Neuro-Oncology program.
Ruham Nasany, MD, is leading a multi-disciplinary team for the new Neuro-Oncology program.
 Satish Krishnamurthy, MD, leads the Neurosurgery department and is a funded researcher. In Fall 2020 he received a $324,000 DOD grant to find a pharmacological solution for hydrocephalus instead of repeated shunt surgery.
Satish Krishnamurthy, MD, leads the Neurosurgery department and is a funded researcher. In Fall 2020 he received a $324,000 DOD grant to find a pharmacological solution for hydrocephalus instead of repeated shunt surgery.
 Robert Beach, MD, monitoring patient Amyee Rodriguez of Gouverneur, New York
Robert Beach, MD, monitoring patient Amyee Rodriguez of Gouverneur, New York Frozen samples of brain cancer tumors can be carefully thawed, put in a nourishing medium and placed in a body-temperature incubator to bring them back to life at Upstate’s Brain Tumor Research Laboratory.
Frozen samples of brain cancer tumors can be carefully thawed, put in a nourishing medium and placed in a body-temperature incubator to bring them back to life at Upstate’s Brain Tumor Research Laboratory.



 Dr. Wickline (center) with Uday Myneni, MS, MBBS, MCH, and his resident team at the first annual arthroplasty conference in Hyderabad, India. Dr. Wickline performed the first anterior hip replacement with the HANA table, televised live to over 400 surgeons.
Dr. Wickline (center) with Uday Myneni, MS, MBBS, MCH, and his resident team at the first annual arthroplasty conference in Hyderabad, India. Dr. Wickline performed the first anterior hip replacement with the HANA table, televised live to over 400 surgeons.