
As both the region’s largest employer and Central New York’s only academic medical center, Upstate Medical University is an important hub of healthcare delivery through its clinical system of two hospital campuses and nearly 70 specialty clinics. Patient centered medical innovation is accelerating in its hospital’s cardiovascular program—which has long established clinical and research activities—to make its major advancements in cardiovascular care available to patients in the region.
“The advancements I’m seeing at Upstate in cardiovascular care are going to make a world of difference for patients in Central New York,” said Amy Tucker, MD, MHCM, Upstate’s Chief Medical Officer. She pointed to the recruitment of Cynthia C. Taub, MD, MBA, Chair of Medicine in 2023 as a major highlight and the start of a new focus for the cardiovascular program. Upstate’s current expansion in Adult Cardiology is one of its core priorities and an anchor of the service line.
“Dr. Taub is a cardiologist of international reputation,” said Dr. Tucker. “She will assume the role of President of the American Society for Echocardiography in July 2026 and is an expert in the use of cardiovascular imaging to support cardiovascular care.”
Dr. Tucker explained that Dr. Taub’s expertise in cardiovascular imaging has helped Upstate become increasingly sophisticated in its diagnostic approaches to cardiovascular disease. Since joining Upstate, Dr. Taub has recruited several highly trained and specialized cardiologists to join the team this year: Adeeb Al Quthami, MD, RPVI, FACC, FSCMR, Ankur Kalra, MD, MSc, FACP, FACC, FSCAI, and Jorge Romero, MD, FHRS, FACC. Combining expertise in advanced electrophysiology, complex valve repair using minimally invasive techniques, and more. “My goal is to continue building a modern, academic cardiovascular service line here at Upstate. When talking about program building, the number one priority for me is the people – we can’t build anything without people,” said Dr. Taub. “We have excellent care here by some of the best experts in the nation. The patients and the community need to know – they don’t have to travel for state-of the-art cardiac care anymore.”
Advanced Treatment for Atrial Fibrillation The arrival of Dr. Jorge Romero as Section Chief of Cardiac Electrophysiology and Director of Cardiovascular Research and Innovation is a prime example of increased convenience and accessibility for patients, bringing cutting edge treatments directly into their community. Dr. Taub noted that she initially connected with Dr. Romero to refer a patient for a procedure that couldn’t be done locally.
The arrival of Dr. Jorge Romero as Section Chief of Cardiac Electrophysiology and Director of Cardiovascular Research and Innovation is a prime example of increased convenience and accessibility for patients, bringing cutting edge treatments directly into their community. Dr. Taub noted that she initially connected with Dr. Romero to refer a patient for a procedure that couldn’t be done locally.
“An anchor of our program is cardiac electrophysiology. Dr. Romero is a nationally and internationally known expert who has led numerous multicenter clinical trials and has created some newer ways of approaching ablations. He’s one of the few fellowship trained experts in epicardial ventricular tachycardia (VT) ablation. Less than 1% of the electrophysiology workforce can perform epicardial VT ablation with finesse, and he’s one of them,” stated Dr. Taub.
Dr. Romero explained that for the past few decades, atrial fibrillation, one of the most common heart rhythm disorders, has been treated in three different ways: rate control medications and anti-arrhythmic medications, each of which often come with potential side effects and complications, and catheter ablation using either radio frequency energy or cryoablation, essentially heating or freezing the tissue. He and his Upstate colleagues are using a new technology called pulsed-field ablation or PFA: A faster and much safer, targeted technique that addresses the source of abnormal heart rhythms, almost eliminating the risk of major complications.
 “Instead of heating or freezing the tissue, we are creating small holes in the cell membrane, called electroporation. The beauty of this technology is that the cardiac muscle is uniquely sensitive. We only need a small dose of energy to eliminate the triggers for atrial fibrillation located in the pulmonary veins of the patient,” Dr. Romero said, which avoids damage to the smooth muscle of the esophagus, phrenic nerves, and other adjacent structures. This has eliminated the risk of atrial esophageal fistula, a deadly complication that used to happen in 0.2% of ablation cases, but which hasn’t occurred in the 800,000 cases of PFA that have been performed so far worldwide. This new, safer technology greatly benefits the older population, mostly over the ages of 70, who are most likely to suffer from atrial fibrillation, offering improved quality of life and reducing longterm risks. Dr. Romero successfully performed Upstate’s first ablation using the Affera Mapping and Ablation System with the Sphere-9 catheter, a multi-purpose catheter not found at any other facility in New York State outside New York city and Long Island.
“Instead of heating or freezing the tissue, we are creating small holes in the cell membrane, called electroporation. The beauty of this technology is that the cardiac muscle is uniquely sensitive. We only need a small dose of energy to eliminate the triggers for atrial fibrillation located in the pulmonary veins of the patient,” Dr. Romero said, which avoids damage to the smooth muscle of the esophagus, phrenic nerves, and other adjacent structures. This has eliminated the risk of atrial esophageal fistula, a deadly complication that used to happen in 0.2% of ablation cases, but which hasn’t occurred in the 800,000 cases of PFA that have been performed so far worldwide. This new, safer technology greatly benefits the older population, mostly over the ages of 70, who are most likely to suffer from atrial fibrillation, offering improved quality of life and reducing longterm risks. Dr. Romero successfully performed Upstate’s first ablation using the Affera Mapping and Ablation System with the Sphere-9 catheter, a multi-purpose catheter not found at any other facility in New York State outside New York city and Long Island.
PFA isn’t the only cutting-edge electrophysiology technology available at Upstate. Other advanced electrophysiology offerings at Upstate include endocardial and epicardial VT ablation, cardiac and renal denervation, radiation therapy to treat ventricular arrhythmias and headless CRT system.
Dr. Romero also discussed the benefits of the Synchronicity clinical trial that’s already available for patients at Upstate. “The Synchronicity trial is going to be a landmark study comparing biventricular pacing versus conduction system pacing (left-bundle branch area pacing) for patients with ischemic and non-ischemic cardiomyopathy who are candidates for cardiac resynchronization therapy. It was recently activated, and we are enrolling patients now,” he said.
Minimally Invasive Cardiovascular Techniques
Another aspect of cardiovascular care at Upstate that offers life-saving technology is in the realm of interventional cardiology. Leading the charge in minimally invasive surgical cardiovascular procedures is Dr. Ankur Kalra, Chief of the Division of Cardiology.
“Dr. Kalra is a very notable interventional cardiologist who is increasing the types of complex procedures we’re able to do here at Upstate,” said Dr. Tucker. “We’re very excited to be able to offer less invasive, but effective, ways of treating valvular heart disease and coronary disease that might have required invasive surgery in the past.”
The transcatheter heart valve procedures Dr. Kalra has expertise in, including transcatheter aortic valve replacement, or TAVR, are important, less invasive alternatives for patients who aren’t candidates for open-heart surgery. Dr. Kalra explained that these procedures involve replacing or repairing heart valves using a combination of wires and catheters, with valves crimped onto a balloon that can pass all the way up to the heart through vessels in the patient’s leg– a small incision compared with open heart surgery, which requires cracking through the breastbone to access the heart. Unlike open-heart surgery, which often requires a multi-day hospital stay, transcatheter heart valve procedures allow patients to return home the next day; in some instances, even the same
day.
 “It’s less morbid; recovery is fast, and outcomes are very similar to open-heart surgery,” said Dr. Kalra. “Transcatheter techniques for the aortic valve are becoming the procedure of choice. Even patients who are at low risk for complications following open heart surgery are eligible for and favor the transcatheter heart valve due to significantly less morbidity following the procedure, and faster return to normal life.”
“It’s less morbid; recovery is fast, and outcomes are very similar to open-heart surgery,” said Dr. Kalra. “Transcatheter techniques for the aortic valve are becoming the procedure of choice. Even patients who are at low risk for complications following open heart surgery are eligible for and favor the transcatheter heart valve due to significantly less morbidity following the procedure, and faster return to normal life.”
Transcatheter techniques also are being used at Upstate to treat patients with heart failure who are optimized on maximally tolerated medical therapy but still have leaky mitral valves. Through a procedure known as mitral transcatheter edge-to-edge repair (mTEER) (Mitral), patients can live longer with less recurrent heart failure, Dr. Kalra explained.
“We offer a comprehensive approach to patients here at Upstate,” stated Dr. Kalra. “We discuss patients as a multidisciplinary heart team that involves their cardiologist, someone like me (structural interventional cardiologist), our surgical colleagues, and cardiologists with expertise in advanced cardiac imaging, and we decide the most comprehensive, evidence-based solution for them. So, the care is individualized, multidisciplinary, and the decisions are shared.”
Enhanced Cardiovascular Imaging
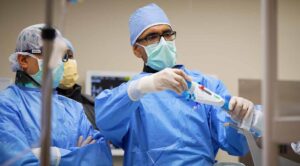 Foundational to cardiovascular care is cardiovascular imaging, which is used not only for visualizing and diagnosing cardiac disease, but also during interventional procedures. Under the guidance of Dr. Adeeb Al-Quthami, Director of Cardiovascular Imaging, significant investments in the latest technology have been secured for the benefit of Upstate’s patients.
Foundational to cardiovascular care is cardiovascular imaging, which is used not only for visualizing and diagnosing cardiac disease, but also during interventional procedures. Under the guidance of Dr. Adeeb Al-Quthami, Director of Cardiovascular Imaging, significant investments in the latest technology have been secured for the benefit of Upstate’s patients.
“Dr. Al-Quthami is truly a talented individual trained in advanced cardiac imaging including cardiac MRI, cardiac CT and nuclear cardiology,” said Dr. Taub. “He’s an expert in treating patients with peripheral vascular disease.”
Cardiac CT (computed tomography) and cardiac MRI (magnetic resonance imaging) technology have advanced significantly in the last 10 years, Dr. Al-Quthami explained.
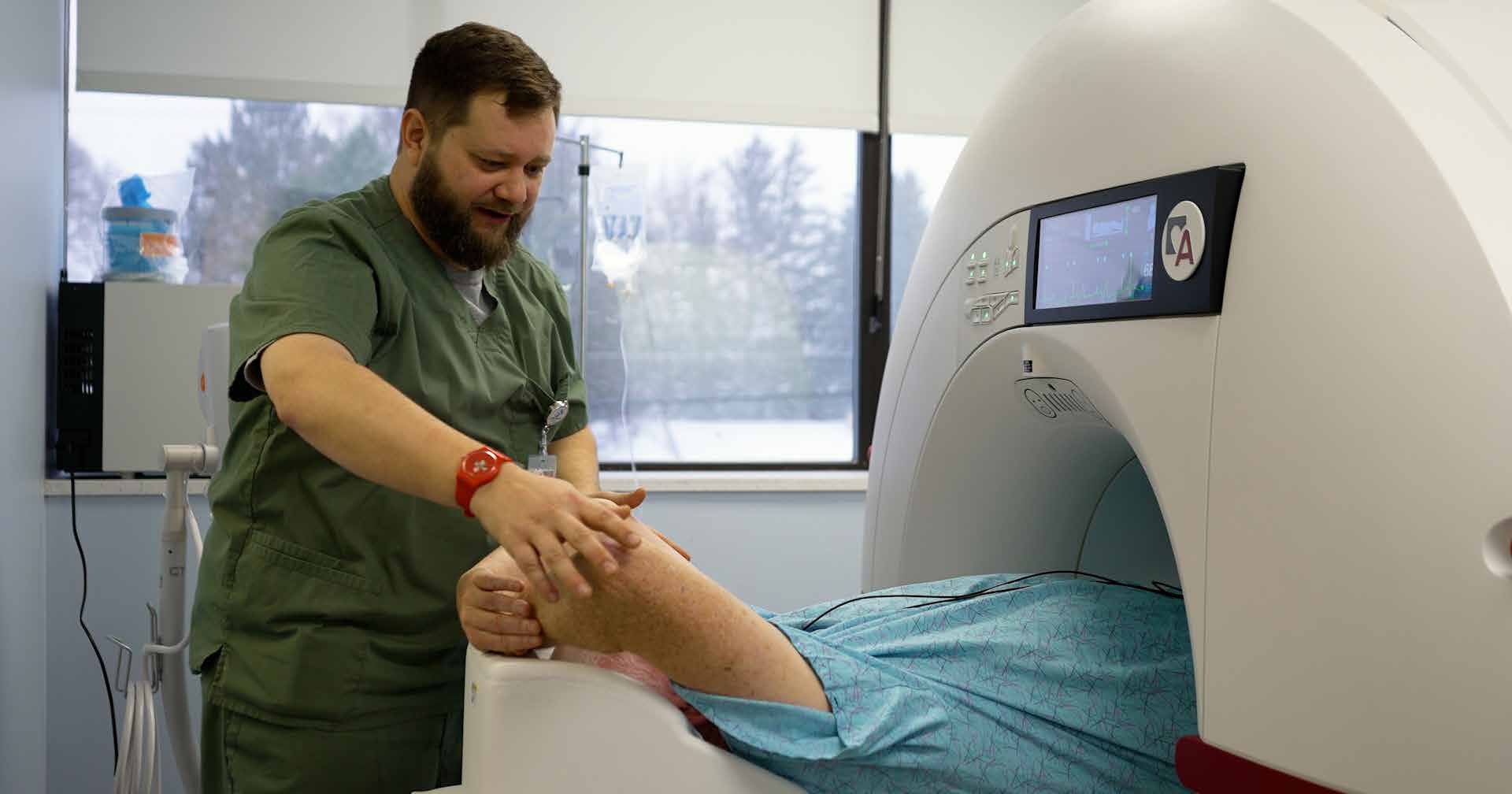 “We can visualize the heart to a very high degree in terms of tiny detail,” he said. “If you try to take a picture of something that’s moving, it’s going to blur, especially if what you’re trying to take a picture of is small. With the advancements in technology, we can take a picture of the heart within a fraction of a heartbeat,” identifying patients’ unique anatomy and offering precise, personalized treatment for each patient.
“We can visualize the heart to a very high degree in terms of tiny detail,” he said. “If you try to take a picture of something that’s moving, it’s going to blur, especially if what you’re trying to take a picture of is small. With the advancements in technology, we can take a picture of the heart within a fraction of a heartbeat,” identifying patients’ unique anatomy and offering precise, personalized treatment for each patient.
 Launched within the last year, AI assisted plaque analysis software, called HeartFlow, is now helping the Upstate cardiovascular team to better assess a patient’s risk for a future heart attack. Dr. Al-Quthami explained how this new technology offers improvement over the traditional coronary calcium scan.
Launched within the last year, AI assisted plaque analysis software, called HeartFlow, is now helping the Upstate cardiovascular team to better assess a patient’s risk for a future heart attack. Dr. Al-Quthami explained how this new technology offers improvement over the traditional coronary calcium scan.
“With the new AI-supported technology, we can look at the entire coronary tree and get a calcium score. But in addition, it gives us the amount of non-calcified plaque, detecting whether these types of plaques are low attenuating or fatfilled plaques. If those reach a certain percentage, the patient is determined to be very high-risk in terms of future heart
attacks,” said Dr. Al-Quthami.
Planning for the Future of Heart Care
 By recruiting more cardiovascular experts to Upstate and continuing to invest in the innovative technologies they use, Dr. Tucker highlighted how the Upstate cardiovascular program is committed to staying at the forefront of cardiovascular care.
By recruiting more cardiovascular experts to Upstate and continuing to invest in the innovative technologies they use, Dr. Tucker highlighted how the Upstate cardiovascular program is committed to staying at the forefront of cardiovascular care.
“We’re really hitting all three tiers of the cardiovascular care continuum: We’re bringing the most cutting-edge technologies to diagnose, we’re bringing in cutting-edge technologies in therapy, and we’re now beginning to offer clinical trials in this space so we can identify the next wave of therapies that may be most impactful for patients,” Dr. Tucker outlined. “So, patients can have a true one-stop shop experience in cardiovascular care without having to travel outside our region.”
As Dr. Tucker explained, these forward looking advancements have garnered enthusiasm and excitement within the entire cardiovascular team. “I see a lot of enthusiasm to learn, to grow, and to continue to push boundaries,” she added. “There is so much insistence on the patient-centered nature of care. That enthusiasm and dedication is palpable, and it makes it an exciting time to be a part of the cardiovascular division here at Upstate.”



 Clinicians hear it every day, stressed patients, and stressed staff. The pressures of changing systems, social media chatter, and a world that seems to be restructuring at every level.
Clinicians hear it every day, stressed patients, and stressed staff. The pressures of changing systems, social media chatter, and a world that seems to be restructuring at every level. When Melanie McNally, MD first began practicing urology, she didn’t anticipate developing a focus on urologic issues specific to women. However, about five years into her practice, she found many women were experiencing urologic health concerns that gynecology was illequipped to manage.
When Melanie McNally, MD first began practicing urology, she didn’t anticipate developing a focus on urologic issues specific to women. However, about five years into her practice, she found many women were experiencing urologic health concerns that gynecology was illequipped to manage. Stallone has held two unwavering truths: he wanted to be a physician, and he wanted to serve his country. Both were anchored by clear purpose.
Stallone has held two unwavering truths: he wanted to be a physician, and he wanted to serve his country. Both were anchored by clear purpose. He went on to earn both an MD and MBA simultaneously from the University of Pennsylvania, and later an MA in National Security Policy Studies from the U.S. Naval War College. He also serves as an Air Force Colonel and has been with the New York Air National Guard for more than 28 years, the past seven as the New York State Air Surgeon. These accomplishments reflect a career built on discipline, leadership, and a breadth of perspective informed by medicine, business, and service.
He went on to earn both an MD and MBA simultaneously from the University of Pennsylvania, and later an MA in National Security Policy Studies from the U.S. Naval War College. He also serves as an Air Force Colonel and has been with the New York Air National Guard for more than 28 years, the past seven as the New York State Air Surgeon. These accomplishments reflect a career built on discipline, leadership, and a breadth of perspective informed by medicine, business, and service. As his career evolved, Dr. Stallone stepped into health system leadership roles, including serving as a hospitalist, physician leader, and former health system CEO, gaining a broader view of how care is delivered and where it often breaks down. He saw firsthand the pressures facing providers, the operational realities behind clinical decisions, and the importance of aligning strategy with real world practice.
As his career evolved, Dr. Stallone stepped into health system leadership roles, including serving as a hospitalist, physician leader, and former health system CEO, gaining a broader view of how care is delivered and where it often breaks down. He saw firsthand the pressures facing providers, the operational realities behind clinical decisions, and the importance of aligning strategy with real world practice. That belief drew him to Excellus BlueCross BlueShield (Excellus BCBS) well before his executive appointment. Through his involvement on the plan’s Central New York and Southern Tier regional advisory boards and governing board of directors, Dr. Stallone developed a deeper understanding of the organization’s nonprofit mission and its commitment to community-focused care. Just as important, he learned the value of listening. “You have to understand providers, the community, payors, and the people doing the work,” he says. “That’s how you design programs that actually make a difference.”
That belief drew him to Excellus BlueCross BlueShield (Excellus BCBS) well before his executive appointment. Through his involvement on the plan’s Central New York and Southern Tier regional advisory boards and governing board of directors, Dr. Stallone developed a deeper understanding of the organization’s nonprofit mission and its commitment to community-focused care. Just as important, he learned the value of listening. “You have to understand providers, the community, payors, and the people doing the work,” he says. “That’s how you design programs that actually make a difference.” At the core of his vision is partnership. Drawing on his experience as both a physician and a former health system CEO, Dr. Stallone sees collaboration as the most effective path forward in an increasingly complex healthcare environment. He designs practical, sustainable, and impactful programs by grounding his strategy in the real challenges facing the healthcare system, including rising costs.
At the core of his vision is partnership. Drawing on his experience as both a physician and a former health system CEO, Dr. Stallone sees collaboration as the most effective path forward in an increasingly complex healthcare environment. He designs practical, sustainable, and impactful programs by grounding his strategy in the real challenges facing the healthcare system, including rising costs.  Dr. Stallone envisions Excellus BCBS as a bridge-builder, bringing together providers, health systems, and community partners to solve problems collaboratively. His focus is on creating pathways that strengthen relationships, improve coordination, and deliver measurable improvements in care—all while staying true to the organization’s mission.
Dr. Stallone envisions Excellus BCBS as a bridge-builder, bringing together providers, health systems, and community partners to solve problems collaboratively. His focus is on creating pathways that strengthen relationships, improve coordination, and deliver measurable improvements in care—all while staying true to the organization’s mission.